RESEARCH & INSIGHTS
ACA & Behavioral Health Provider Survey Results
How behavioral health practices are experiencing the ACA subsidy expiration — in their own data
Celeriti Practice Management | Ethan Sena | March 2026
In February 2026, Celeriti Practice Management surveyed 80 behavioral health practices to understand how the expiration of ACA enhanced subsidies is affecting their operations, their patients, and their outlook. These are the results.
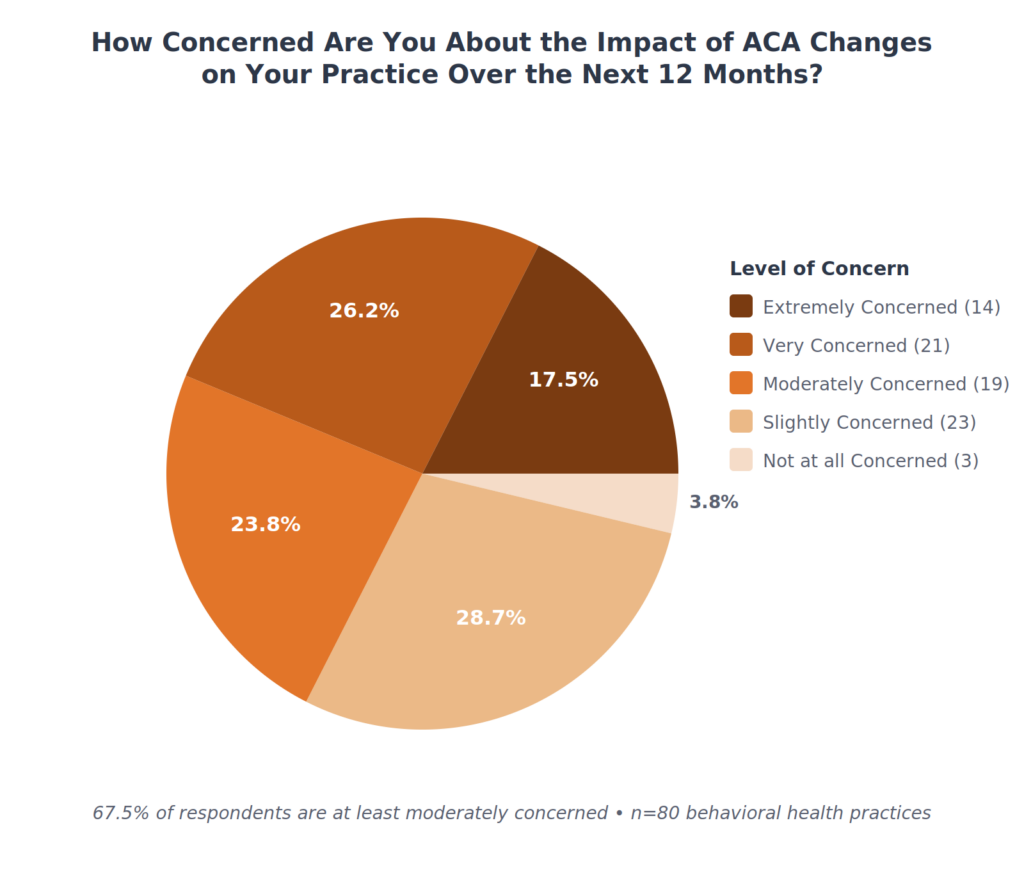
Level of Concern
When asked how concerned they are about the impact of ACA changes on their practice, 67.5% of respondents reported being at least moderately concerned. Only 3.75% said they are not concerned at all.
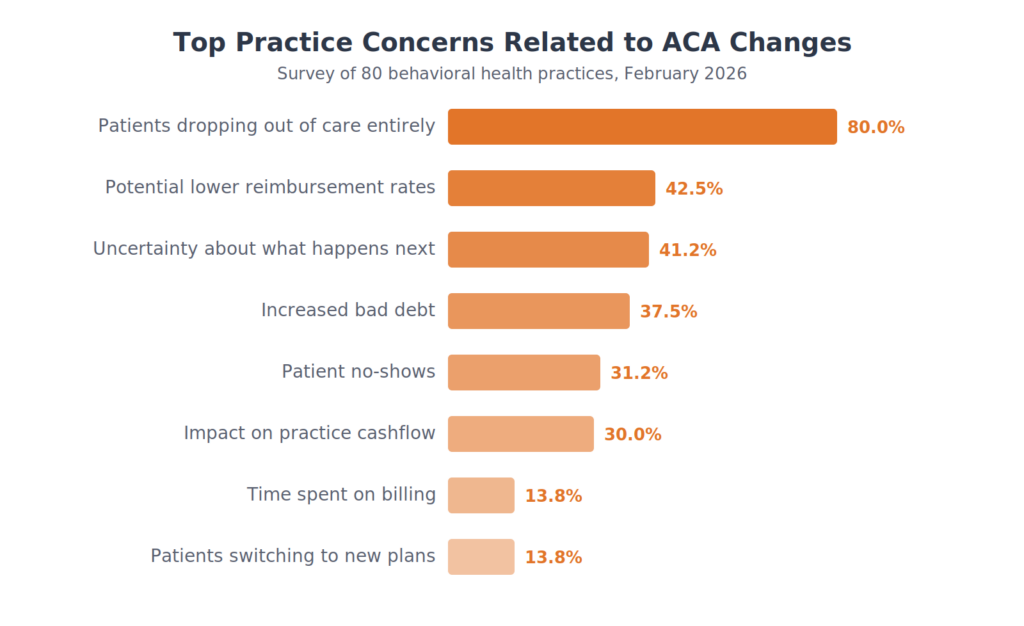
Top Practice Concerns
Respondents were asked to select their biggest concerns related to ACA changes. Patient dropout dominated, with 80% citing it as a top concern — nearly double the next highest response.
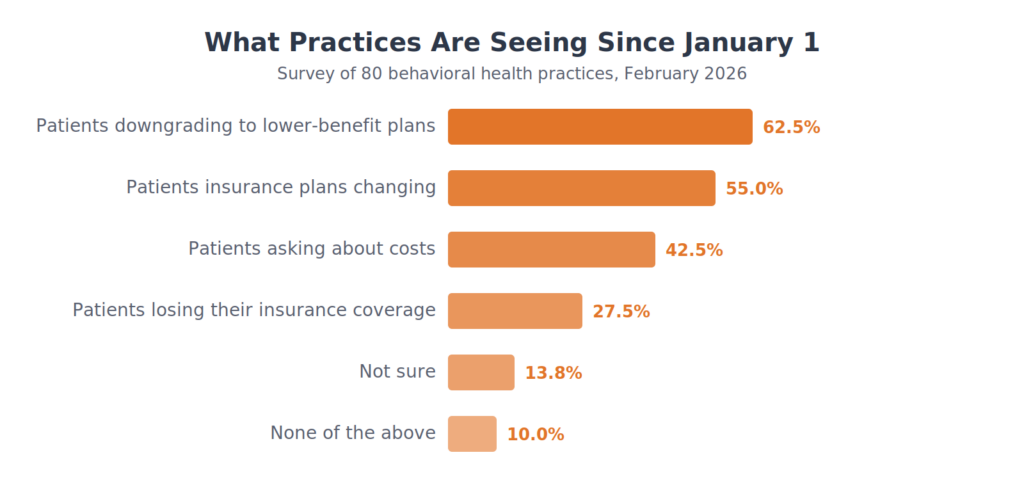
What Practices Are Seeing
Practices reported the changes they have observed since subsidies expired. The most common: patients downgrading to lower-benefit, higher-deductible plans.
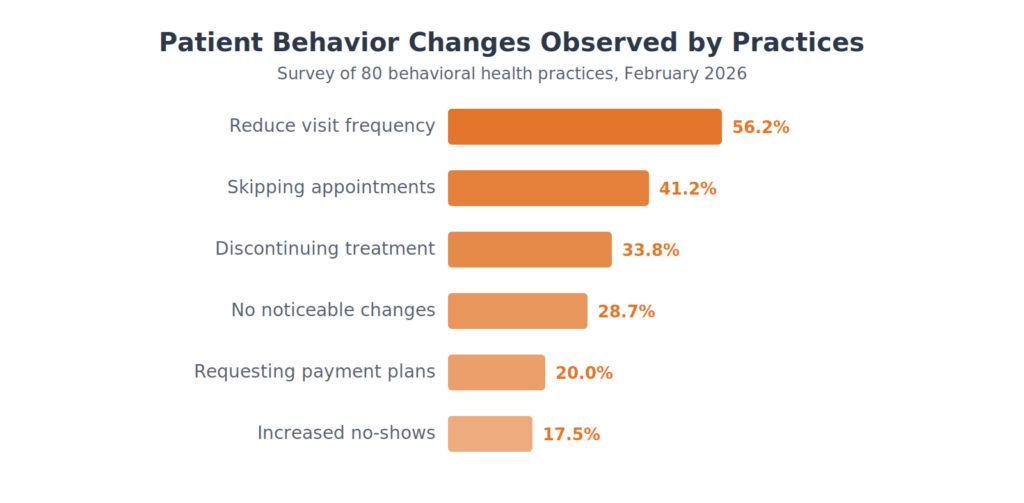
Patient Behavior Changes
Beyond insurance-level changes, practices are seeing direct shifts in how patients engage with care. Over half report patients asking to reduce visit frequency.
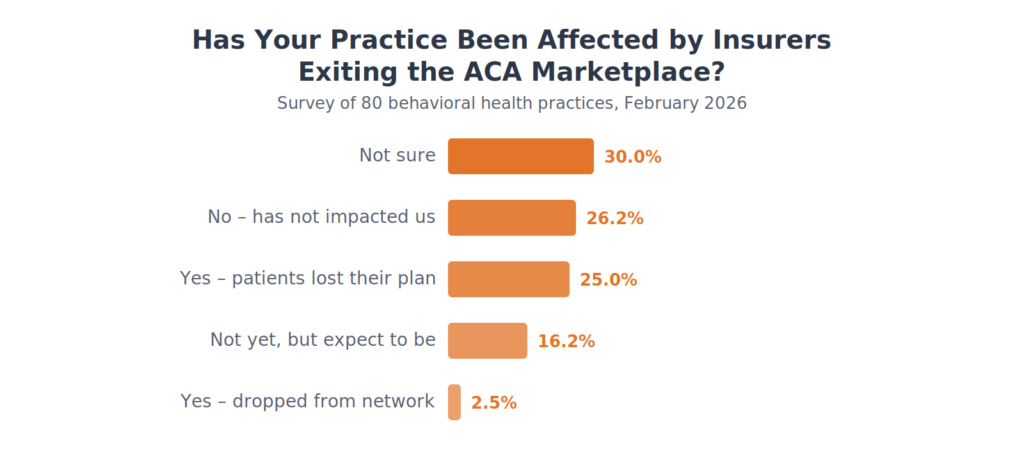
Insurer Exit Impact
Major insurers like Aetna/CVS have exited ACA markets in multiple states. Practices were asked whether this has affected them directly.
Methodology + Resources
This survey was conducted February 9 – 20, 2026, by Celeriti Credentialing & Practice Consulting. 80 behavioral health practices responded. Respondents were asked about their level of concern, observed changes since January 1, 2026, patient behavior shifts, and the impact of insurer exits from ACA marketplaces. All questions allowed multiple selections except for level of concern.
